
Earlier this year, the Institute for Safe Medication Practices (ISMP) in conjunction with the U.S. Pharmacopeia (USP) published a comprehensive list1 of drug names creating the most confusion.
The list features nearly 1,600 drug names and includes both brand names and generic names. Of course, what’s unsettling about this list, besides its length, is that more and more drugs are being added each year, despite the fact that the FDA reviews over 4002 proposed names annually, of which it rejects one third for issues such as looking or sounding like another drug.
25 Drug Names That Need a Second or Third Look
All of the drugs on the ISMP list have been reported to the FDA’s MedWatch Adverse Event Reporting System as having been confused with other drugs2. However, some drugs are confused more often than others, according to the State University of New York (SUNY) Department of Pharmacy Services.3
Such is the case with Risperidone (an antipsychotic) and Ropinirole (dopamine agonist), two drugs that resulted in MedWatch receiving 226 reports of drug confusion, as well as multiple hospitalizations because of mix-ups, in just one year.4
These two drugs, along with 23 others featured in our top 25 list are in need of serious medical attention in order to prevent disaster.
|
DRUG NAMES |
ISSUES POTENTIALLY CREATED BY MIX-UPS |
|
1. Novolin 2. Novolog 3. Novolin 70/30 |
Hypoglycemia, poor diabetes control and other serious issues |
|
4. Clonidine 5. Clonazepam |
Hypotension, seizures and other serious issues |
|
6. Ambisome 7. Abelcet 8. Amphocin |
Respiratory arrest, renal failure and death |
|
9. Metformin 10. Metronidazole |
Hypoglycemia or untreated infection |
|
11. Vinblastine 12. Vincristine |
Death |
|
13. Tramadol 14. Trazodone 15. Toradol |
Decline in pain control, changes in psychiatric symptoms and other serious issues |
|
16. Hydroxyzine 17. Hydralazine 18. Hydrochlorothiazide |
Sedation, hypotension and other serious issues |
|
19. Hydromorphone 20. Morphine |
Death |
|
21. Celebrex 22. Cerebyx 23. Celexa |
Mental decline, lack of pain control, seizures and other serious issues |
|
24. Risperidone 25. Ropinirole |
Confusion, lethargy, ataxia, hallucinations, dizziness and other serious issues |
A Growing Margin of Medication Error
Currently, the FDA states that 10 percent of all medication errors are a result of drug name confusion. However, this statistic is based on the number of anonymous reports received by the MedWatch and most believe this estimate to be extremely conservative due to underreporting. In fact, in an interview5 with the Patient Safety Authority (PSA), Carol A. Holquist, R.Ph., the Director of Medication Errors and Technical Support in the FDA's Office of Drug Safety said, "Medication errors are not usually due to incompetence, but they are underreported because people are afraid of the blame." PSA believes the actual percentage of medication errors due to drug name confusion is more likely around 25 percent.6
>> See Game On: Check Your Brain’s Ability to Avoid Medication Mistakes
Eliminating the Potential for Error
From the moment a prescription is written, to the time a drug is dispensed, drug errors can occur at any point of interaction, and are caused by a number of issues including similar names, abbreviations, acronyms, dose designations packaging and labels; illegible handwriting; and new and unfamiliar drug names. To prevent drug confusion the FDA has specific recommendations for everyone who handles drugs:
- Manufacturers — Spell drug names using both upper- and lowercase letters (TALLman Lettering) to highlight differences in similar names.
- Doctors — Write both brand and generic names on prescriptions; print drug names in block letters instead of cursive writing; refrain from using abbreviations; include the reason for the drug on the prescription.
- Pharmacists — Keep look-alike, sound-alike products separated from one another on pharmacy shelves. Verify information that is not clear with doctors before filling a prescription.
Although the FDA has not made official recommendations for preventing drug name confusion to hospitals, it is widely known that many hospitals are moving toward automated medication management, such as RFID tags, to eliminate error, saves lives, as well as time and money.
>> See What is RFID
Consider the workflows for procedural and emergency kit and tray management in the hospital pharmacy, comparing the current manual process vs. utilizing an automated RFID solution for the same task:
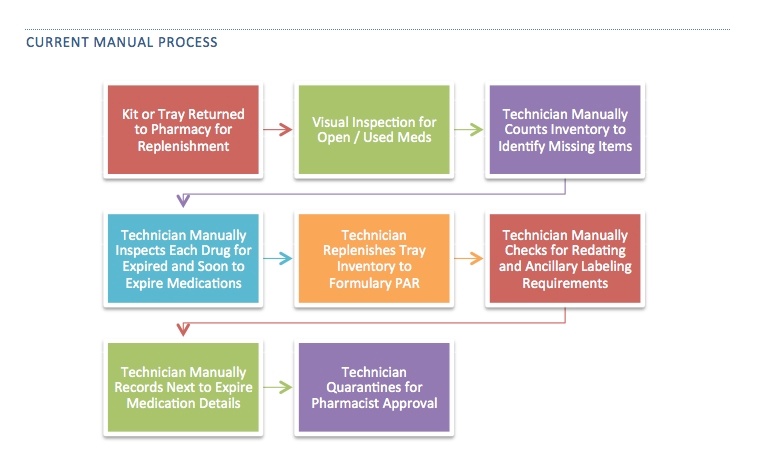
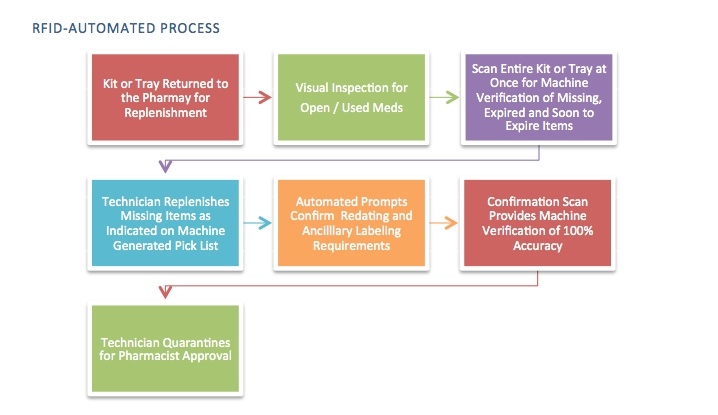
Note that in the RFID-automated process, machine verification compares what it’s the tray with the approved formulary for that tray and generates a pick list. Then, once the tray is replenished, it is scanned again for accuracy – if there is any missing or an unexpected (wrong drug) in the tray, the RFID system alerts the user to fix the error and reconfirm before processing can continue.
>> See Intelliguard® Kit and Tray Management System
Any manual process that relies on human perfection is ripe for error – and in the pharmacy, that can mean the difference between healing, pain control and even survival. Isn't it time to address drug names creating confusion and errors?
We recently compiled research around why and how errors happen and discovered some interesting facts. If you haven’t downloaded it already, check out our white paper: The Risk of Relying on Human Perfection and see how RFID can help remove human error contributors and give you confidence that you are provided the safest, quality care to patients.
Sources:
1 https://www.ismp.org/tools/confuseddrugnames.pdf
2 http://www.medicinenet.com/script/main/art.asp?articlekey=53208&page=4
3 http://www.downstate.edu/patientsafety/Look_alike_Sound_alike_drug_list.pdf
4 http://www.fda.gov/drugs/drugsafety/ucm258805.htm
5 http://www.medicinenet.com/script/main/art.asp?articlekey=53208
6 http://patientsafetyauthority.org/ADVISORIES/AdvisoryLibrary/2004/dec1(4)/Pages/07.aspx

